t is widely recognised that achieving good patient flow in an acute hospitals is a daily struggle. We believe that one of the main principles of achieving good patient flow is to ensure patients get what they need, when they need it, i.e. on time and in full. The Improvement Academy has been working with a team at Hull and East Yorkshire Hospitals to develop and test an intervention which encompasses this principle.
Timed Action Plans for Patients (TAPPs) is an intervention which:
- supports the planning of a patient’s care, ensuring each action is allocated a time scale for completion;
- considers the actions that are required to take the patient through to their planned discharge date;
- creates a visual prompt for staff, making it clear what needs to happen on each day of the patients stay;
- allows for actions and planned discharge dates to be reviewed daily and modified if required; and
- collects detailed information about each delay within the patient’s journey.
Ultimately TAPPs is a tool which improves quality and safety through supporting the delivery of consistent and reliable patient care. When patients get what they need, when they need it, they spend less time waiting and a measureable outcome for this is a reduction in length of stay. Through reducing delays, patients are less likely to come to harm through acquiring a hospital acquired infection, having a fall, or suffer deterioration associated with a hospital stay for frail, elderly patients. We are currently evaluating TAPPs to learn its full impact.
Impact
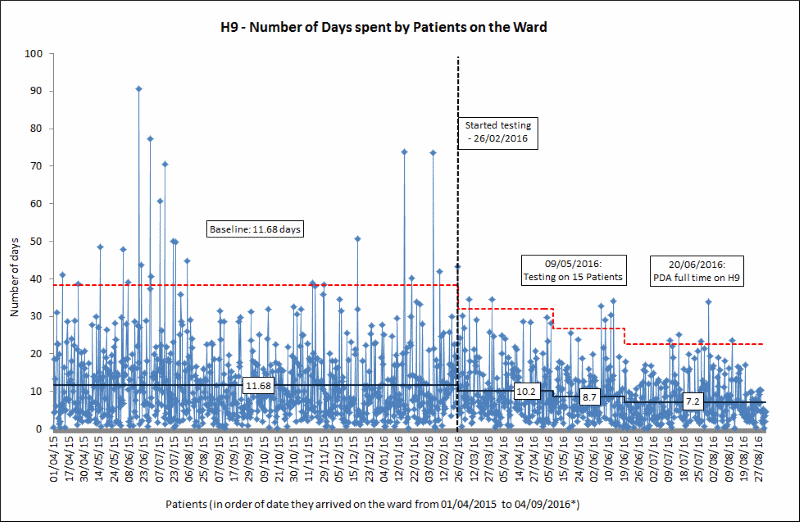
Since we started developing and testing TAPPs with Ward 9 at Hull Royal Infirmary we have seen a reduction in length of stay from a baseline of 11.68 to 7.5 (as of 04/12/2016), saving an estimated 3,301 bed days.
There has been a corresponding increase of 47% in the number of discharges and transfers from the ward, allowing the team to treat an extra 291 patients.
Kay Brighton, Sister on Ward 9 (pictured opposite with Dr Fiona Thomson), says ‘surprisingly, although we are seeing more patients on the ward, it doesn’t feel busier; in fact it feels calmer as everyone is clear about what needs to happen to get our patients home’.
During our testing of TAPPs, the ward has also being developing and expanding the role of their Patient Discharge Assistant (PDA), who is now a full time member of the team. Through using TAPPs the team is able to plan discharge arrangements earlier, helping to fully utilise the PDA role.
Future Plans
We will continue to work with Hull and East Yorkshire Hospitals Trust to fine tune TAPPs as we extend the use of TAPPs to all of the patients on Ward 9 and as we do this we will spread the use of TAPPs to other wards so we can begin to see the effects at hospital level.
We recognise that the presence of a tool like TAPPs does not automatically guarantee that it will be used, or that patient flow is high on the list of clinical and ward staff’s priorities. Therefore, we have started to, and will continue to, uncover the barriers and facilitators to achieving patient flow, using the Achieving Behaviour Change for Patient Safety Toolkit.
We will be using the information collected though using TAPPs to identify which are the major causes of delay and looking at ways to make improvements in order to make the biggest impact on patient flow.
Other hospitals are expressing interest in testing TAPPs in their ward environments too.




