Seclusion refers to the supervised confinement and isolation of a patient, away from other patients, in an area from which the patient is prevented from leaving, where it is of immediate necessity for the purpose of the containment of severe behavioural disturbance which is likely to cause harm to others.” (ref: NHS Patient Safety Thermometer).
The use of seclusion is fraught with the risk of various adverse effects for both patients and staff. It is an intervention that is generally disliked by the patients and staff that use it. The desire to reduce the use of seclusion is a priority for many health care providers particularly in light of least restrictive practice principles and the reduction of known mental health patient safety harms including, the use of restraint and violence and aggression (ref: NHS Patient Safety Thermometer).
The Yorkshire & Humber Academic Health Science Network (AHSN) Improvement Academy, have been working with one low secure, male, acute admission ward to reduce the use of seclusion within its service through, amongst other things, the introduction of safety huddles and a de-briefing process.
What have we achieved?
The following statistical control chart shows sustained improvement in the number of seclusion episodes on the test ward.
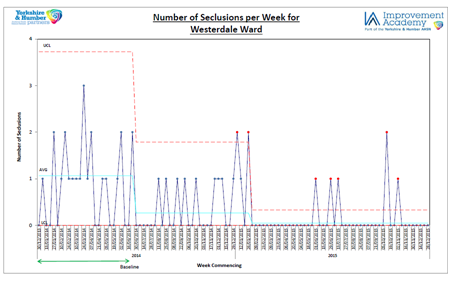
Outputs include:
- 2015 seclusion figures identified a reduction in the number of seclusions since 2014 from 31 episodes in 2014 to 13 in 2015 which is a 58% reduction and a reduction in the repeated episodes of patients requiring seclusion from 7 repeated episodes to 2 repeated episodes, a 71% reduction.
- Patient Safety Huddles have been established on the ward and are held daily to identify patients at risk of seclusion and plan care accordingly.
- A debriefing process is being developed to identify lessons learnt from a seclusion event should it occur. This process includes the development of a patient feedback survey and has used the outcomes of a literature search to inform the process created.
- Action learning sets, have been established for band 6 nurse clinical leads.
- A regional round table event in October 2015 aimed at frontline staff working in services that have seclusion facilities, or care for people in isolation to the main ward environment. The event aimed to: reduce the use of seclusion in their services Improve care delivery, encourage least restrictive practice Improve patient experience and improve patient safety and reduce harm.
- The event led to the Department of Health co-ordinating a meeting with a lead from the Care Quality Commission (CQC), the Improvement Academy (IA) project lead and ward manager to discuss what seclusion is and the impacts of the differing interpretations of what constitutes seclusion, leading to:
- To support the consistency of CQC assessment of seclusion during inspections, a video has been developed to support the awareness and understanding of inspectors as to the different ways in which services users may be secluded e.g. understanding that a service user does not have to be in a designated, locked seclusion room / suite in order to be secluded and that even though a service may not have a seclusion “room” they may still be secluding service users.
- The ward concerned, IA project manager and CQC and DOH to plan, develop and facilitate an event to explain and disseminate the above work and to demonstrate; the origins of the concept, a case study for improvement and to describe solutions on moving forward.


Safety huddles and de-brief process
- To find out more about the Safety Huddles process click here
- To find out more about the seclusion de-brief process click here
Future plans:
- Increase networks and communication between other mental health inpatient services.
- Review and develop safety huddles and de-brief process.
For further information please contact project lead Lyndsey Charles.




